|
"In a word, describe how you feel right now."
I recently saw this question asked in a 99,000-member fibromyalgia support group. Almost all the 377 answers just two days after the post had negative connotations. Words like exhausted, defeated, overwhelmed, afraid, lousy, anxious, depressed, painful, lifeless, restricted, broken, irritable, lost, done, and disconnected were shared. The few positive answers included words like confident, grateful, proud, and hopeful. The overwhelming percentage of negative words saddens me about the level of pain care and what people living with pain are experiencing. My answer was confident. However, there was a time in my journey with chronic pain when my answer wouldn't have been as positive. That was before I attended a pain rehabilitation program, accepted the pain, and learned to live well despite it using active self-management strategies. We need to stop treating chronic pain as prolonged acute pain because it's not prolonged acute pain. It is its own condition. Clinicians need to empower people living with pain – shifting from a "find-it, fix-it" mentality to a "self-management" mentality. Learn more
If you have chronic pain, the answer is probably yes.
As acute pain becomes chronic, it’s often less about structural damage and more about an over-sensitized nervous system maintained by maladaptive neuroplastic changes over time – putting your nervous system in a state of high reactivity. Central sensitization is associated with the development, maintenance, and amplification of chronic pain. It changes how the brain processes pain – misfiring nerve signals and continuing to tell the body it hurts. The official definition of central sensitization by the International Association for the Study of Pain is, “Increased responsiveness of nociceptive neurons in the central nervous system to their normal or subthreshold afferent input.” In other words, you become more sensitive to pain and other sensory stimuli – causing more pain more often. You may feel it when only lightly touched or bumped. You may feel it in different areas of the body other than the spot of the original injury. You may also have different types of feelings like achiness, stabbing, tingling, or burning, for example. Features of central sensitization have been identified in nearly all chronic pain conditions, no matter the underlying cause. Some of the conditions it has been tied to include fibromyalgia, whiplash, headaches, shoulder pain, osteoarthritis, chronic fatigue syndrome, non-cardiac chest pain, irritable bowel syndrome, TMJ, neuropathic pain, complex regional pain syndrome, spinal back pain, pelvic pain, inflammatory conditions like rheumatoid arthritis, and post-cancer pain. Changing it The good news is we can change our nervous system. Central sensitization can be reversed by doing things that promote positive neuroplasticity like changing how we think about pain, react to pain, and manage pain. The best treatment is a biopsychosocial approach, including pain education, physical therapy, cognitive behavioral therapy, pain acceptance, sleep management, and pharmaceutical management. I got a heavy dose of all these at the Mayo Clinic Pain Rehabilitation Center. Learn more
Self-management tools 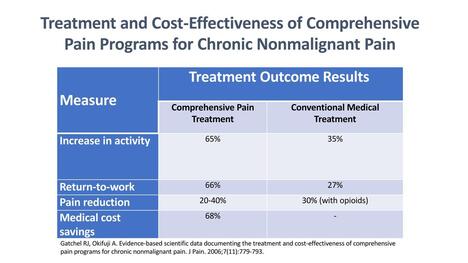 If biomedical treatments like medicines, rest, supplements, ice, heat, injections, and physical therapy didn’t resolve pain when it was acute, is it reasonable to expect using only the same treatments to change our symptoms when the pain becomes chronic? It's not. We must change the paradigm. Pain is more than a biomedical condition. We need to treat both mind and body. As Dr. Rachel Zoffness reminds us, " Because pain is biopsychosocial, treatment must be, too." Comprehensive pain treatment that addresses the biopsychosocial aspects of a person's pain experience is not only more clinically effective than conventional medical treatment by itself, it’s also more cost-efficient. Acute pain vs. chronic pain There are two types of pain: acute and chronic. Acute pain is the body’s normal response to tissue damage or injury. The pain matches the damage and treatment works - lasting less than three months. Chronic pain is an abnormal response, becomes its own disease/condition, and doesn’t improve over time. It can happen long after an injury or illness heals. Treatments don’t always work or stop working and symptoms can change and grow over time. The longer we have pain, the less likely it is related to tissue damage or injury and the better our bodies can become at creating it and turning up the pain volume. It’s a process known as central sensitization. Sensitization can happen in all chronic pain conditions, no matter the underlying cause, including fibromyalgia, whiplash, shoulder pain, neuropathic pain, chronic fatigue syndrome, non-cardiac chest pain, irritable bowel syndrome, temporomandibular disorders, post-surgical pain, complex regional pain syndrome, low back pain, osteoarthritis, pelvic pain, and headache. This 22-minute video from Dr. Sletten with the Mayo Clinic Pain Rehabilitation Center (PRC) does an awesome job explaining pain and sensitization, why traditional medical treatments don’t always work for chronic pain, and their approach at the PRC. I encourage you to watch it. Learn more
Pain is the body’s alarm system. It’s designed to protect us from danger just like a home security system or a smoke detector. It’s the body’s normal response to acute tissue damage or injury and heals in normally 3-6 months.
But what happens when pain doesn’t go away? Once pain persists beyond the normal healing time, it becomes chronic - losing its warning function and becomes its own disease/condition. It’s an abnormal response (with or without obvious pathology). Although all pain hurts, not all pain indicates damage. We know what to expect from our pain by the very nature of it being chronic or ongoing. It’s not like getting burnt, twisting an ankle, or getting stung by a bee that needs protection until the injury has heals. Of course, any unexpected new pain should be investigated. Learn more
|
Categories
All
Archives
July 2024
CHRONIC PAIN CHAMPIONS, LLC AND THIS WEBSITE DOES NOT PROVIDE MEDICAL ADVICE
All information is for educational purposes only. Use at your own risk. By accessing/using this website and any related pages/information/products/services, you agree to the terms and conditions. PLEASE SEE THE DISCLAIMER PAGE TO LEARN MORE. ©2024 Chronic Pain Champions, LLC All rights reserved. For personal, non-commercial use. |
